Introduction
Mycoplasma are small, simple bacteria which lack a cell wall and resistant to many common antibiotics such as penicillin and streptomycin. Once infect, they can induce changes to the cell cultures, including altered growth rates, morphological changes, chromosomal aberrations, and altered cell metabolism. Thus, contamination of mycoplasma is a major problem in cell culture technology.
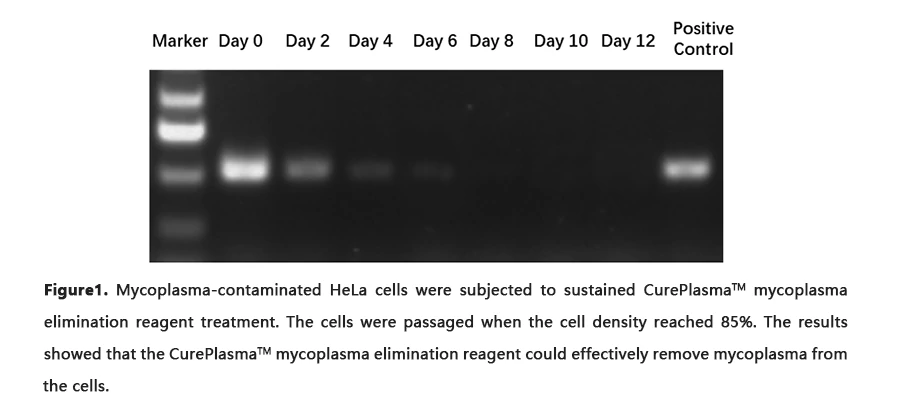
Many cell lines infected by mycoplasmas have been successfully treated with CurePlasmaTM, including hybridomas, lymphocytes, epithelial cells, murine embryonic stem cells, and retrovirus packaging cells. It has been shown that treatment with CurePlasma restores cellular responses following mycoplasma clearance(Figure1).
Click here to purchase Cureplasma™ Mycoplasma Elimination Reagent
An Introduction to Cell Contamination and Mycoplasma Elimation
Content
1. Cell culture and cell contamination
Cell culture is the process by which cells are grown under controlled conditions, generally outside their natural environment. Life science research using cell cultures has resulted in numerous improvements to the treatment of human disease. In addition, with the advent of stem cell technology, cultured cells are themselves becoming therapeutics. In this light, cell culture contamination could be one of the biggest hindrances to scientific progress today.
Cell contaminations are not restricted to occasionally detected infections with bacteria, yeast, or fungi originating from unsterile cell culture technique, but also comprise hidden infections with slowly growing bacteria, various viruses, and cross-contaminating eukaryotic cells from other cell cultures that are not evident during routine cell culture monitoring. Of these, according to ATCC, mycoplasma contaminations exhibit the highest prevalence, with more than 20% of infected cultures. Mycoplasma can alter a great variety of cellular characteristics and often leads to experimental artefacts and spurious results.
2. Mycoplasma contamination
Mycoplasmas are the smallest free-living organisms and considered to be the simplest of bacteria. They belong to the bacterial class Mollicutes, whose members are distinguished by their lack of a cell wall and their plasma-like form. The first strains of mycoplasma were isolated at the Pasteur Institute in 1898, and to date, 20 of the roughly 190 known species have been identified as bona fide contaminants of laboratory cell cultures. Owing to their extremely basic genomes, mycoplasmas must function as parasites in order to meet their energy and biosynthesis demands.
Given their tiny size (typically less than one micrometer), mycoplasma contamination are undetectable by the naked eye or even by optical microscopy; thus, they typically go undetected for extended periods of time. Moreover, given their lack of a cell wall, they are resistant to many common antibiotics such as penicillin and streptomycin. Hundreds of mycoplasmas can attach to a single eukaryotic cell, eventually invading the host by fusing with the cell membrane. Upon entry into the cell, mycoplasmas multiply, eventually outnumbering host cells by 1000-fold, and they circumvent host defenses to survive.
Mycoplasma can compete with host cells for biosynthetic precursors and nutrients and can alter DNA, RNA and protein synthesis, diminish amino acid and ATP levels, introduce chromosomal alterations, and modify host-cell plasma membrane antigens. A microarray analysis on contaminated cultured human cells has revealed the severe effects that mycoplasmas can have on the expression of hundreds of genes, including some that encode receptors, ion channels, growth factors and oncogenes. Moreover, mycoplasmas contain highly immunogenic lipoproteins anchored on the outer face of the plasma membrane. These lipoproteins are recognized by specific pattern recognition receptors on immune cells-in particular, Toll-like receptor 2 (TLR2). Upon recognition of mycoplasmal lipoproteins, TLR2 induces the NF-kB pathway, which leads to activation of these cells and consequently, to biased experimental results.
Based on studies by FDA, ATCC, and others, it is estimated that 11% to 15% (or more) of all cell cultures today are contaminated with mycoplasma. The most common source of mycoplasma contamination in cell culture research is another previously infected culture brought into the laboratory. Another major source is the laboratory worker as human mycoplasma continues to be a major source of mycoplasma contamination in cell culture. Mycoplasma contamination can be best prevented by a strict policy of quarantining all incoming cell lines until testing has confirmed the absence of mycoplasma. Besides, routine test for mycoplasma contamination is recommended for all laboratories carrying out cell culture whether in-house or contracted out. There are several assured ways of detecting mycoplasma contamination, including fluorescent staining,
ELISA, PCR, immunostaining, autoradiography, or microbiological assays.
3. Mycoplasma detection
Working with authenticated cell lines free from mycoplasma contamination is a prerequisite for the generation of robust, reliable, and reproducible data in the biomedical research field. It is always a good practice to check cell lines on a regular basis for mycoplasma contamination. The difficulty in controlling a particular contaminant is often related to its ease of detection. Most bacterial and fungal contaminations will cause the medium to turn cloudy and quickly kill the cells in culture. However, mycoplasmas are undetectable by the naked eye or even by optical microscopy.
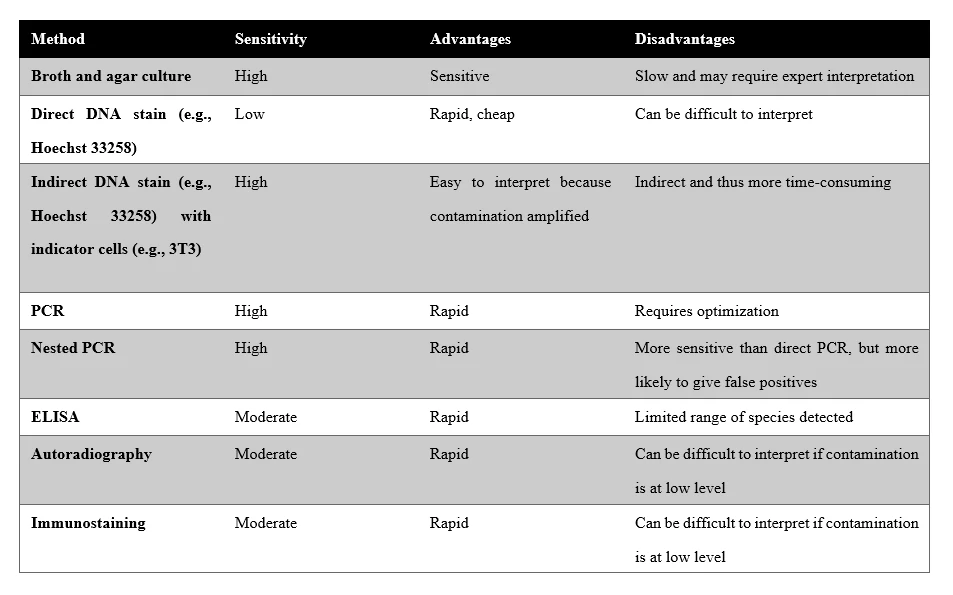
Nowadays, there are a number of mycoplasma tests available, each with its own advantages and disadvantages. The full selection of mycoplasma detection kits available make the tedious ongoing process of mycoplasma test much more efficient and less worrisome. The three most popular methods for mycoplasma detection include mycoplasma culture, DNA staining method and PCR.
a) Agar-and-broth procedure
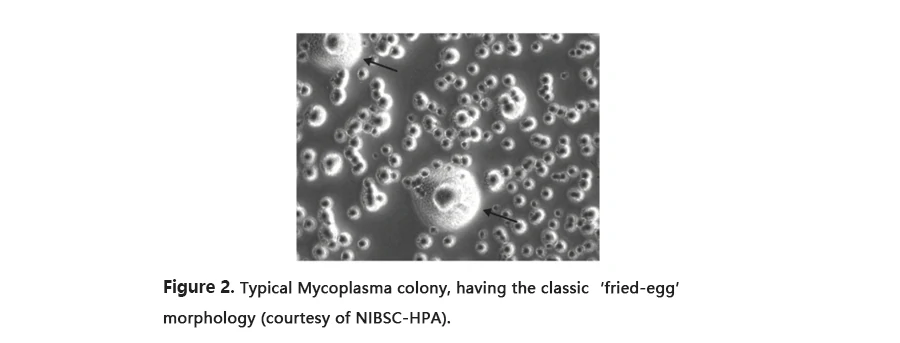
For a long time, microbiological cultivation in broth and subsequently on agar, also known as the agar and broth procedure, was regarded as the most sensitive and specific mycoplasma test and was commonly used as the reference method (the “gold standard”). In this test, a sample of the suspected cultures is added to agar plates that have been set up as absolute mycoplasma heaven. The idea is to give them everything they could ever want, so that any mycoplasma contamination present in the cell culture at the time of sampling will grow and be readily apparent on agar test plates (Figure3). However, it takes a month to obtain the result. Moreover, the mycoplasma detection reagents, like medium, are complex with a relatively short shelf-life and live positive controls must be included.
 b) DNA detection
b) DNA detection
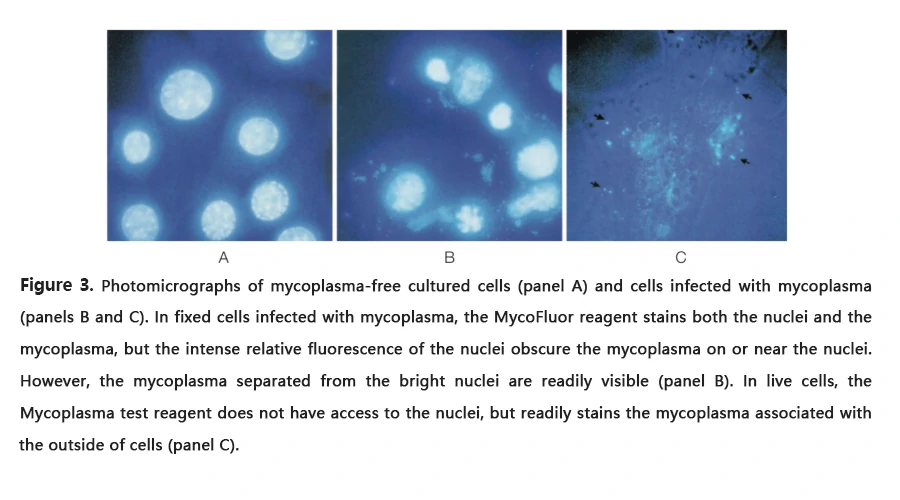
The DNA staining method of mycoplasma detection takes several days, because one have to grow a sample of the suspected cell cultures with indicator cells – usually Vero cells, which have a large cytoplasmic area. Cells are then stained for DNA with a fluorescent dye (such as Hoechst dye), and mycoplasmas that present in the cell sample will be visible as fluorescent spots, or granules, surrounding the nucleus of the indicator cells. A benefit of this method is that it detects the mycoplasma strain M. hyorhinis, which is not reliably detected by the gold-standard culture isolation method.
 c) PCR method
c) PCR method
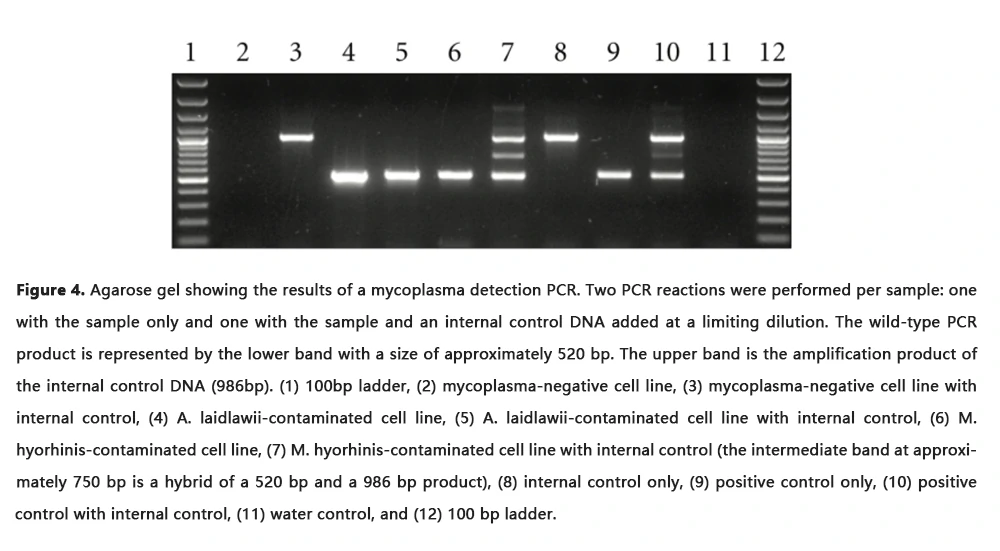
Polymerase chain reaction (PCR) provides a very sensitive and specific option for the direct detection of mycoplasmas in cell cultures. Comparison of the PCR method with other well-established assays (DNA/RNA hybridization, microbiological culture) showed that the PCR assay is a very robust, efficient, and reliable method for mycoplasma detection. Thus, detecting mycoplasma by PCR amplification is recommended by The American Type Culture Collection (ATCC) and nucleic acid amplification technique (NAT) is now accepted by FDA as a compendial method for Mycoplasma detection.
The choice of the primer sequences is one of the most crucial decisions. Several primer sequences are published for both single and nested PCR and with narrow or broad specificity for mycoplasma or eubacteria species. In most cases, the 16S rDNA sequences are used as target sequences, because this gene contains regions with more and less conserved sequences. This gene also offers the opportunity to perform a PCR with the 16S rDNA or an RT-PCR (reverse transcriptase–PCR) with the cDNA of the 16S rRNA.
 d) Enzymatic and ELISA methods
d) Enzymatic and ELISA methods
Other forms of mycoplasma detection are also available. In the enzymatic method, you add a sample of your suspected cell culture to a substrate that converts ADP to ATP in the presence of mycoplasmal enzymes. The Mycoplasma test reagent also contains another compound that functions as a read-out, such as the enzyme luciferase, which uses the ATP to produce light - signaling the presence of mycoplasma infection in your cultures. Another alternative detection strategy relies on the widely-used ELISA format, which can indicate the presence of mycoplasma using either antibodies, or labeled probes for the mycoplasma’s 16S rRNA genes.
4. Mycoplasma elimination
The sources of mycoplasma contamination in the laboratory are very challenging to completely control. As certain mycoplasma species are found on human skin, they can be introduced through poor aseptic technique. Additionally, they can come from contaminated supplements such as fetal bovine serum, and most importantly from other contaminated cell cultures. Once mycoplasma contaminates a culture, it can quickly spread to contaminate other areas of the lab. Strict adherence to good laboratory practices and routine testing for mycoplasma is highly recommended for successful mycoplasma removal.
Once mycoplasmas have been detected, the best solution to eliminate them and to prevent them from spreading is to discard the contaminated cell line. However, valuable cell lines that are too precious to be sacrificed can be salvaged by treatment with effective mycoplasma elimination reagents, including mycoplasma-selective antibiotics. These mycoplasma treatment reagent have been shown to eliminate mycoplasma and to restore cell behavior and responses within days or weeks after treatment. Till now, there are three classes of antibiotics that kill mycoplasma when used at relatively low concentrations: tetracyclines, macrolides and quinolones. Tetracyclines and macrolides block protein synthesis by interfering with ribosome translation, whereas quinolones inhibit replication of mycoplasma DNA.
Generally, there are four different approaches to the treatment of infected cell cultures with antibiotics: (1) the use of a single antibiotic compound (e.g., the fluoroquinolones), where basically the same procedure is employed for each antibiotic of that group; (2) the simultaneous application of two different antibiotics; (3) the use of a combination therapy applying two antimycoplasma agents subsequently in alternating cycles; and (4) the use of a membrane-active peptide to get rid of the majority of the mycoplasmas present in the medium and on the cells, followed by the application of an antibiotic to eliminate the remaining mycoplasmas inside and outside the cells. Based these idea, many mycoplasma removal kits comprised of different mycoplasma removal reagents are currently on the market.
CurePlasma is a single ready-to-use mycoplasma elimination reagent that can be added directly to the culture medium. The two antibiotics in CurePlasma have distinct mechanisms: one blocks protein synthesis and the other stops DNA replication. Therefore, CurePlasma is more effective at removing mycoplasma and prevents the generation of resistant strains. Moreover, in contrast to other mycoplasma removal reagent, CurePlasma is active against free as well as intracellular forms of mycoplasma. It ensures that, following mycoplasma treatment, cell cultures do not become re-infected by mycoplasma that had previously been released from the intracellular compartments of infected cells. To date, no consistent or permanent alterations that affect eukaryotic cells during or after CurePlasma treatment have been reported.

 b) DNA detection
The DNA staining method of mycoplasma detection takes several days, because one have to grow a sample of the suspected cell cultures with indicator cells – usually Vero cells, which have a large cytoplasmic area. Cells are then stained for DNA with a fluorescent dye (such as Hoechst dye), and mycoplasmas that present in the cell sample will be visible as fluorescent spots, or granules, surrounding the nucleus of the indicator cells. A benefit of this method is that it detects the mycoplasma strain M. hyorhinis, which is not reliably detected by the gold-standard culture isolation method.
b) DNA detection
The DNA staining method of mycoplasma detection takes several days, because one have to grow a sample of the suspected cell cultures with indicator cells – usually Vero cells, which have a large cytoplasmic area. Cells are then stained for DNA with a fluorescent dye (such as Hoechst dye), and mycoplasmas that present in the cell sample will be visible as fluorescent spots, or granules, surrounding the nucleus of the indicator cells. A benefit of this method is that it detects the mycoplasma strain M. hyorhinis, which is not reliably detected by the gold-standard culture isolation method.
 c) PCR method
Polymerase chain reaction (PCR) provides a very sensitive and specific option for the direct detection of mycoplasmas in cell cultures. Comparison of the PCR method with other well-established assays (DNA/RNA hybridization, microbiological culture) showed that the PCR assay is a very robust, efficient, and reliable method for mycoplasma detection. Thus, detecting mycoplasma by PCR amplification is recommended by The American Type Culture Collection (ATCC) and nucleic acid amplification technique (NAT) is now accepted by FDA as a compendial method for Mycoplasma detection.
The choice of the primer sequences is one of the most crucial decisions. Several primer sequences are published for both single and nested PCR and with narrow or broad specificity for mycoplasma or eubacteria species. In most cases, the 16S rDNA sequences are used as target sequences, because this gene contains regions with more and less conserved sequences. This gene also offers the opportunity to perform a PCR with the 16S rDNA or an RT-PCR (reverse transcriptase–PCR) with the cDNA of the 16S rRNA.
c) PCR method
Polymerase chain reaction (PCR) provides a very sensitive and specific option for the direct detection of mycoplasmas in cell cultures. Comparison of the PCR method with other well-established assays (DNA/RNA hybridization, microbiological culture) showed that the PCR assay is a very robust, efficient, and reliable method for mycoplasma detection. Thus, detecting mycoplasma by PCR amplification is recommended by The American Type Culture Collection (ATCC) and nucleic acid amplification technique (NAT) is now accepted by FDA as a compendial method for Mycoplasma detection.
The choice of the primer sequences is one of the most crucial decisions. Several primer sequences are published for both single and nested PCR and with narrow or broad specificity for mycoplasma or eubacteria species. In most cases, the 16S rDNA sequences are used as target sequences, because this gene contains regions with more and less conserved sequences. This gene also offers the opportunity to perform a PCR with the 16S rDNA or an RT-PCR (reverse transcriptase–PCR) with the cDNA of the 16S rRNA.
 d) Enzymatic and ELISA methods
Other forms of mycoplasma detection are also available. In the enzymatic method, you add a sample of your suspected cell culture to a substrate that converts ADP to ATP in the presence of mycoplasmal enzymes. The Mycoplasma test reagent also contains another compound that functions as a read-out, such as the enzyme luciferase, which uses the ATP to produce light - signaling the presence of mycoplasma infection in your cultures. Another alternative detection strategy relies on the widely-used ELISA format, which can indicate the presence of mycoplasma using either antibodies, or labeled probes for the mycoplasma’s 16S rRNA genes.
d) Enzymatic and ELISA methods
Other forms of mycoplasma detection are also available. In the enzymatic method, you add a sample of your suspected cell culture to a substrate that converts ADP to ATP in the presence of mycoplasmal enzymes. The Mycoplasma test reagent also contains another compound that functions as a read-out, such as the enzyme luciferase, which uses the ATP to produce light - signaling the presence of mycoplasma infection in your cultures. Another alternative detection strategy relies on the widely-used ELISA format, which can indicate the presence of mycoplasma using either antibodies, or labeled probes for the mycoplasma’s 16S rRNA genes.





